Best VATS Thoracoscopic Surgery in Ludhiana Punjab
Best VATS Surgery in Ludhiana, Punjab (India)
Dr. Atul Misha is a world-renowned surgeon for VATS (Video Assisted Thoracoscopic surgery) in Ludhiana, Punjab, India.
Dr Atul Mishra, Professor & Unit Head, Dayanand Medical College & Hospital, LudhianaHis hospital is equipped with the latest technology. Dr. Atul has a great team of doctors working under him to treat the patients suffering from various diseases of chest and thorax.
Dr Mishra has pioneered advanced VATS procedure and is the first surgeon to start this procedure in the whole of North India. He is performing all the VATS procedure viz. lobectomy, Bullectomy, Pleurodesis, thymectomy, empyema surgery
and so on.
He has been doing VATS since 2004, and till now has done more than 2000 VATS procedures with excellent results
VATS has a plethora of benefits over the open surgery, which a surgeon would recommend depending on the medical condition of the patient. It has now become a very common surgery, which has been used in daily practices by not only Dr. Atul Mishra, but by all the reputed surgeons across the globe.
Dr. Atul is a trained surgeon who shares a very high success rate in performing Best VATS Surgery in Ludhiana, Punjab and Thoracoscopic surgery in India. If we go for the surgery reports then most people who underwent VATS found it beneficial and had no complications post their surgery. Moreover, the surgery is also associated with a lower risk of arrhythmias, reintubation, blood transfusion when it’s compared to open surgery. VATS has shown long-term positive outcomes and is chosen by people over open surgery due to its multiple benefits.
VATS (Video Assisted Thoracic Surgery)
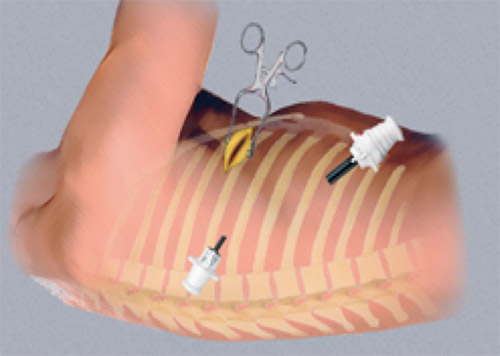
VATS is a keyhole or minimally access surgery of chest. In this surgical technique a small video camera called thoracoscope is put into the chest through a small cut to see inside and perform surgery using special long fine instruments through two or three small cuts (0.5 – 1cm). The thoracoscope transfers the image of inside of chest cavity onto a High Definition monitor. Surgeon performs operation by viewing the monitor.
Other names of VATS are thoracoscopy, Thoracoscopic surgery or pleuroscopy.
There are two lungs in our body which supply oxygen (O2) to the body and remove carbon dioxide (CO2).
We can remove a part of lung (lobectomy) or even whole of one lung (pneumonectomy) without causing any change in O2 and CO2 balance because the other remanant lung expands and takes over the function of the removed lung.
Advantages of VATS
In VATS we make very small incisions causing very less injury as compared to traditional open surgery in which we make a very long incision (15 to 20 cm), cut the muscles and separate the ribs which can sometimes lead to fracture. As a result of increased trauma, incidence of early and long term pain and discomfort are significantly high in open surgery. So patient undergoing minimally invasive VATS procedure experience
Less pain after surgery
Reduced bleeding during surgery
Shorter operation time
Less chance of infection after surgery
Shorter hospital admission
They recover more quickly and soon return to work (starting to earn there livelihood)
Less incidence of long term (chronic) pain and shoulder dysfunction
Better quality of life
The skin incision is small so more cosmetic scar
You can watch a video of VATS lobectomy performed by Dr Atul Mishra on our YouTube Channel:
youtube.com/wyoutu.be/4thoMT0jAws
YOU CAN SUBSCRIBE OUR CHANNEL TO WATCH MORE ACADEMIC SURGICAL VIDEOS :
Indications and types of VATS procedures
VATS Lobectomy
When a large part of lung is removed by minimally invasive technique it is called VATS lobectomy.
It is commonly done to treat:
Lung Cancer
Fungal infection of lung (Aspergilloma) with bleed (Hemoptysis)
Hydatid cyst
Tuberculosis
Pneumonia (Necrotizing infection/ abscess)
Bullous lung disease with pneumothorax (air in pleural cavity)
Congenital conditions (Sequestration)
Wedge resection
Surgical removal of a triangular-shaped portion of tissue from lungs to diagnose or treat a lump in lung
Lung biopsy
A small part of lung tissue is removed by VATS technique to diagnose the disease. The tissue is used for pathological and microscopic examination to see for lung infection, interstitial lung disease or cancer
Drainage of pleural effusion
A pleural effusion is collection of fluid between the two layers of the pleura (the thin membrane that covers the lung and interior surface of chest wall). The common causes of fluid accumulation are infection (Tuberculosis, Pneumonia), cancer, heart disease, liver damage and kidney failure. Thoracoscopically we can remove this fluid which is causing breathing difficulty by compressing the lung. We can prevent recollection of fluid (recurrence) by instilling sterile talc or an antibiotic in the chest cavity.
Mediastinal, Pericardial and Thymus thoracoscopic procedures
The mediastinum is the middle part of chest cavity between the two lungs.
The area around the heart covered by a membrane is called the pericardium.
The thymus is a small gland present in the upper and front part of mediastinum.
With the help of VATS we can examine mediastinum or pericardium, remove a part of tissue for diagnostic purpose (biopsy) or surgically remove a benign or malignant (cancerous) growth.
Thymus can be removed (Thymectomy) in a patient of Myasthenia Gravis or thymic tumors (Thymoma)
Other conditions where VATS is useful:
Esophageal diseases
Hiatus hernia repair
Surgery to relieve excessive sweating in palm and foot(Hyperhydrosis) – Thoracic Sympathectomy
Surgery to relieve Gastro esophageal reflux disease (GERD) (Heart burn)
Treating hernia of Diaphragm or paralysis of diaphragm (eventration)
Diagnostic Test done before VATS surgery
Blood Test
Pulmonary function test (Breathing Test)
CT Scan
ECG
EMPYEMA THORACIS : VATS DECORTICATION
Empyema also called pyothorax is a disease in which pus collects in the area between the lungs and the chest wall. This space is called as the pleural space. Pus is a fluid that is filled with immune cells, dead cells and bacteria. It can cause the surface of lungs and chest cavity to stick together and form pockets. Lungs are not able to expand completely leading to difficulty in breathing.
Causes
Empyema usually occurs as a complication of pneumonia which is an infection of lung . The common types of bacteria causing this infection are Streptococcus pneumonia and staphylococcus aureus.
Empyema is very common seen in patients suffering from tuberculosis.
Sometimes empyema can occur after surgery of chest or chest trauma.
Risk Factors
Patients with following conditions are at more risk of getting empyema-
Bronchiectasis
Chronic obstructive pulmonary disease (COPD)- chronic bronchitis and asthma
Rheumatoid arthritis
Alcohol
Diabetes
Poor immune system
Lung abscess
Symptoms
Difficulty in breathing
Dry cough
Fever
Increased perspiration
Chest pain (stabbing)
Headache
Confusion
Decreased appetite
Empyema can be simple or complex.
Simple Empyema-
It occurs in early part of disease with freely flowing pus
Complex empyema-
Occurs in late stage when scar tissue converts the chest cavity into multiple smaller spaces called as loculation. If the infection continues for long it can lead to the formation of a thick peel over the lung preventing it from expanding during breathing. Surgery is required to free it so that it can function normally
Diagnosis
Chest X-Ray
Ultrasound chest
CT scan of chest
Blood Test – White blood cell count, C-reactive protein, culture of bacteria
Needle aspiration –Needle inserted through back of rib cage to take sample of fluid to look for bacteria
Treatment
Aim of treatment is drainage of pus and treating infection with antibiotics.
Drainage of pus –
Simple case- Needle can be used to remove the pus (Thoracocentesis)
Complex empyema-
These patients require putting drainage tube to remove the pus (Tube thoracostomy)
LUNG CANCER IN INDIA
Current Status
Lung cancer has reached an epidemic proportion. There has been 30 – 40% increase in lung cancer over last decade. All cancers including lung cancer is on rise and the reasons are – control of communicable diseases, increased life expectancy, increase in total population, adoption of cancer associated life style (like smoking, physical inactivity, westernized diet), urbanization, industrialization, radiation, air pollution, water pollution and so on.
Among all cancer, lung cancer is most common cause of cancer death with a figure of 20%. Every year 63 000 people die from lung cancer. Estimated incidence of lung cancer in India is 70 000 per year, 5.6 per 100 000 population.
In India lung cancer occurs in young age group with about 40 % occurring in less than 50 years of age.
80% of lung cancer patients come from rural area which may be due to increased rate of bidi smoking and pesticide exposure. Most cancers in rural area are diagnosed in advanced stage.
Lung cancer is rising in females and non smokers also. 9 out of 10 cases are diagnosed in last stage.
Not much we have achieved in controlling lung cancer which is clearly shown by marginal improvement of 5 year survival of lung cancer from 5% in 1950 to 14% IN 1994 in contrast to other cancer where it is 52%.
CAUSES OF INCREASE IN LUNG CANCER
Almost 90% of patients with lung cancer have history of active smoking or tobacco use in other form. Tobacco smoke contains over 4000 chemical compounds, many of which have been shown to be causing cancer or carcinogenic like Nitrosamine and polycyclic aromatic hydrocarbons. Smoking can narrow the air passage and make breathing difficult and over the course of time destroy lung tissue and trigger changes in cancer.
Every year 60 lac people die directly from use of tobacco out of which 10% i.e. 6 Lacs due to second hand smoking.
There has been alarming rise of lung cancer among females and non smokers. The reasons are-
1. 2nd hand smoking. People who live with smoker have 24% more chance of developing lung cancer.
2. Air Pollution ( 5% of lung cancer occur due to air pollution)
a) Domestic coal/wood burning for cooking purpose is significant factor for lung cancer in non smoking females. Coal smoke contains Radon and Thoron gas.
b) Air pollution from vehicle, industry and power plant can raise the likelihood of developing lung cancer.
c) Exposure of diesel exhaust to truck driver, toll booth worker, rail road worker, garage worker etc.
d) Exposure to radon gas which is produced by breakdown of uranium in soil and rock
3. Occupational exposure to Asbestos in insulation worker and shipyard worker, Arsenic, Uranium and Nickel also lead to increase chance of lung cancer.
4. Lack of micronutrient in diet
Symptoms of Lung Cancer
A new cough that does not go away
Coughing of blood
Shortness of breath
Chest pain
Hoarseness of voice
Loosing weight
Bone pain
Headache
Repeated chest infection
Lung cancer in 1/4th cases are silent and do not cause any symptom.
Incidentally diagnosed on X-Ray or CXT scan done for other purpose.
Diagnostic test for lung cancer
Chest X- Ray is the most common first diagnostic test.
CT Scan
PET Scan- helps in deciding whether a lesion is cancerous or not.
Sputum cytology
Bronchoscopy and biopsy : Visualizing the airways through a thin fiberboptic probe through the nose or mouth may reveal areas of tumor that can be sampled (Biopsied)
Needle biopsy : Fine needle aspiration through the skin, most commonly done under ultrasound or CT guidance useful in retrieving cells for diagnosis of tumor nodule in lung.
Thoracocentesis of fluid in chest for cancer cells
VATS biopsy
Staging
The stage of cancer is a measure of the extent to which cancer has spread in the body. It is important to decide treatment of cancer.
Stage 1 : Confined to lung
Stage 2 & 3 : Outside lung but in the chest
Stage 4 : outside chest spread
Chest X- Ray and sputum test can be done in every hospital and cheap. Other tests only in tertiary care or referral hospital. They are expensive. Government should subsidize there charges and make them available widely to every section of society in private hospitals and free in government hospitals.
Early diagnosis of lung cancer
Low dose CT scan annually in current or former smoker between ages 55 and 80 with at least 30 pack year history of cigarette smoking or who have smoked cigarette within the past 15 years. If we smoke one packet cigarette ever day for one year it is one pack year.
The lung cancer screening techniques increase the likelihood of detection of smaller earlier and curable lung cancer.
Three year of LDCT has decreased lung cancer death by 20%.
Early diagnosis allows curative surgical treatment for the patient with permanently getting rid of the disease. Furthermore we can offer Minimally invasive, keyhole surgery.
Most of the patients in our society in general are afraid of any surgery and they keep on visiting a physicians in search of medical treatment even for clear cut surgical conditions. The reasons for this is fear of big cut on their body, pain, long hospital stay, big scar causing disfigurement, log term disability after surgery, inability to go back to work, can they become normal after surgery?
All these issues are very well addressed by minimally invasive surgery. So if we screen the high risk population and diagnose lung cancer in early stage, these patients can get benefits of keyhole surgery.
Treatment of Lung Cancer
It involves surgical removal of the cancer, chemotherapy or radiation therapy.
Surgery for stage 1 & 2 . The cancer which has not spread beyond lungs. 10 – 35 % of lung cancers can be removed surgically.
Depending on the size of tumor.
Surgeon may remove a portion of lobe (Wedge resection), Remove one lobe
(lobectomy), or entire lung may be removed (Pneumonectomy)
Chemotherapy is giving drugs that stop the growth of cancer by killing cancer cells.
With advancement, treatment options include surgical procedures like VATS (Video Assisted Thoracic surgery) a form of minimally invasive keyhole surgical technique used to diagnose and treat diseases of chest. It can be used to treat and manage the complications of lung cancer too.
Role of VATS in Lungs Cancer
VATS is a keyhole technique to surgically treat lung lesions by making small cut on the chest through which a tiny camera and fine surgical instruments are inserted into the chest wall. The camera transmits image of the inside of the chest into high definition video monitor guiding the surgeon in performing any procedure in the chest and lungs.
Benefits of VATS in Lungs Cancer
It is done with small incision so it causes less pain, early recovery and more cosmetic scar. Surgery is performed more precisely as better well illuminated magnified vision is there in VATS. There is less blood loss, shorter hospital stay, early recovery, early return to work and start earning there livelihood. Very less breathing problem and better quality of life after surgery.
Causes of delay in diagnosis
It starts with patient himself at first level
Lag of time from symptom onset to first visit with primary physicians.
The reasons are :
1. Not taking symptoms seriously
2. No body to escort
3. Long distance
4. Financial reason
5. Family commitment/ marriage in family
6. Fear of death, fear of cancer, denial
-Delay at second level: At primary physician level (upto 5 -6 months delay)
The reasons are:
1. Symptomatic treatment
2. Empirical anti tubercular treatment
3. Miss diagnosis by primary physician : TB, Infection or asthma
In India there is general tendency among physicians to empirically diagnose Tuberculosis more commonly then cancer due to high endeminicity and shortage of facility to confirm cancer like CT scan or bronchoscopy.
Unfortunately the Tuberculosis control program advises physicians to commence empirical ATT for patients with lung shadows that does not resolve with antibiotics treatment.
Remedy for improvement in Early detection
1. Health education and counseling of general public
2. Sensitizing primary physician for timely referral to avoid the situation where curable disease becomes incurable.
3. Increase in facility and availability of diagnostic test at small center to diagnose lung cancer early.
How to prevent lung cancer
Don’t smoke / stop smoking
Avoid second hand smoking
Avoid carcinogen at work (mask)
Eat diet full of fruits and vegetables
Exercise regularly
Make your home and car smoke free
Avoid exercise outdoor on bad air days
Personal hygiene
Radiation control
Control of air pollution
Legislation for tobacco, alcohol and air pollution
Nicotine gums and sprays may be helpful to people trying to quit smoking
Screening to early diagnose and treat lung cancer
Tips to keep lung healthy
1. Exercise
2. Get regular health check up
3. Breathing exercise
4. Maintain good posture
5. Stay hydrated
6. Laughing is a good exercise
7. Be active
8. Prevent infection (frequent hand wash, Good oral hygiene,)
EVENTRATION OF DIAPHRAGM : VATS Plication
In eventration the paralyzed diaphragm muscle remain in an elevated position and prevents normal expansion of the lung with inspiration. The VATS plication procedure flattens the dome of the muscle bringing it to normal inspiratory position. This allows the lung to expand fully improving ventilatory function. Although this procedure does not result in physiological movement of diaphragm but it does reverses the paradoxical motion during inspiration.
VATS (Video Assisted Best Thoracoscopic Surgery in INDIA) Plication
VATS is less invasive, key hole surgery technique, using small incision on chest wall to visualize the diaphragm with camera.
Myasthenia Gravis – Role of Surgical Treatment – VATS Thymectomy
Myasthenia Gravis (MG) is a neuromuscular disease that results in weakness in the skeletal muscles, which are the muscles our body uses for movement. Weakness associated with MG typically increases with more physical activity and gets better with rest. Symptoms include difficulty in talking, problems walking up stairs or lifting objects, facial weakness, breathing difficulty, difficulty in swallowing or chewing, fatigue, change in voice, drooping of eye lids and double vision.
Treatment options:
Medicines like steroid & immunosuppressing drugs can be used . Additionally, cholinesterase inhibitors such as pyridostigmine are also useful for improving communication between nerve & muscles.
Surgery:
Thymus gland removal (Thymectomy), which is part of the immune system, is very effective for many patients with MG. Once the thymus gland is removed patient gets improvement in muscle weakness. Surgery is a safe alternative with high rate of complete improvement and good long-term effect. Thymectomy can be done by minimally invasive (keyhole) technique called as VATS (Video Assisted Thoracoscopic Surgery).
Advantages of VATS:
The advantages of minimal access (Keyhole) technique called VATS are minimal chest injury, less pain and complication after surgery. It allows very early recovery and quick return to work with better cosmetic effect and improved postoperative lung function.
Lifestyle changes to overcome MG :
Must take plenty of rest to help in decreasing muscle weakness. Avoid stress and exposure to hot atmosphere as it can worsen symptoms. For double vision can wear eye patch.
Results are better in young patients (10-55 years) with generalized symptoms, short duration of disease, hyperplastic thymus, more severe symptoms and a high antibody titre.